Medicine Containing Bisphosphonates Bisphosphonates are a group of drugs commonly used in the treatment of osteolysis and in preventing cancer cells from spreading to the bone. Suitable forms for intravenous and oral administration are available. Intravenous bisphosphonates are used to prevent cancerous cells from spreading to the bones, while oral bisphosphonates are commonly used for the treatment of bone osteolysis. There is an important side effect of bisphosphonate-based dentistry that is particularly relevant to the jaw surgeon. The risk of developing osteonecrosis (dead bone tissue) in the jaws after surgical procedures (tooth extraction, dental implant, etc.) in patients using such drugs is high. If you are using these medicines, you should absolutely inform your physician about your condition before proceeding. Your doctor will refer you to your doctor who recommends you to use a bisphosphonate first and to ask if your medicine can be discontinued to reduce the risk of osteonecrosis before any surgical procedures that must be performed. Secondly, you will start antibiotics 3-4 days before you perform surgery and will perform the procedure under these conditions. You need to continue antibiotics after the procedure. Despite these precautions, if dead bone tissue occurs, it must be removed surgically. Depending on the size and location of the dead bone tissue, the operations performed may vary from simple to difficult. If you are using bisphosphonate derivative drugs, you should definitely share this with your physician before dental procedures. Distraction Osteogenesis
It is possible to extend the jaws and jaw bones by surgical procedures when necessary. Extension can be performed within certain limits. In these operations, movements in the soft tissue with bone movement are not sufficient and undesirable conditions such as the emergence of the moved bone piece or aesthetic problems may occur. For this purpose, distraction osteogenesis procedure is used for simultaneous extension of bones with soft tissue.
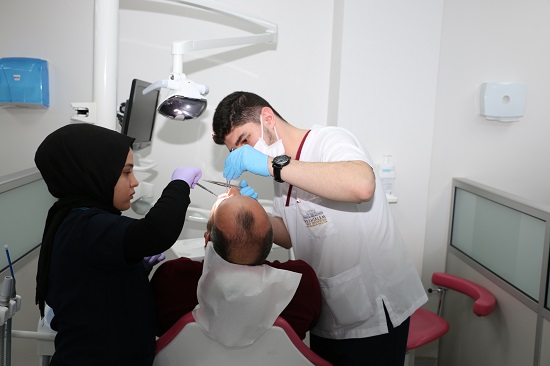
This procedure consists of the insertion of the device to provide extension following the cut made in the desired bone (Osteotomy Prayer), the expectation of new bone formation (Latent Phase) between the incised bone surfaces, the periodic extension of the bone (Distraction Prayer) and the consolidation phase expected to mature the extended new bone. Extension can be made up to 30% of the bone size desired to be extended.
Distraction devices can be placed within the mouth or outside the mouth, depending on the anatomy of the bone to be extended and the amount of bone. With distraction osteogenesis, the patient remains at the hospital, and the final result is achieved sooner. However, devices placed in the osteotomy environment need to be removed with a new surgical procedure after the consolidation phase. This is the disadvantage of this process.
Cleft Lips
Children with lips-and-mouths may have a number of problems that require the care of doctors in different disciplines throughout their care. Nowadays, many hospitals in many countries are bringing doctors in different branches together to establish a lip-palate team. All the experts in such a team are cooperating with the treatment during the development of the lips palate. This kind of team approach provides a wide range of care that meets the child's familial, social, emotional, physiological and educational needs.
Surgical treatments can be planned in 4 different age groups:
- Newborn-12 months
- 1-5 years
- 5-13 years
- 13-18 years
Newborn-12 months
All newborn babies are examined by a pediatrician in the hospital. If the child is born with a cleft lip and / or palate, the pediatrician usually asks the baby to be examined by a plastic surgeon or mouth, teeth and jaw surgeon. Cleft lip and palate feeding and respiration may be problematic. The timing of cleft lip and palate treatment may vary from surgeon to surgery. In general, the lip and then the palate should be treated surgically if available. It is thought that the optimal treatment timing of lip slits should be between 0-6 months. However, for the lip slit to be treated surgically, the weight of the child should be at least 4.5 kg, the blood hemoglobin value at least 10 g / dl and the child should be at least 10 weeks old. A short time after birth, a feeding plate is being made by orthodontists in order for the child to be able to feed properly during the time until the lip surgery is performed. Thus, negative pressure between the lips and the breast can be provided for the child's mothers to breastfeed, and there is no problem in feeding.
When the child is in a suitable situation, the lip repair is done surgically and an appropriate aesthetic appearance and function can be provided for both the parents and the child.
In general, palate clefts can be repaired between 18 and 24 months when speech begins. Today, due to modern anesthesia and asepsis, antisepsis, broad spectrum antibiotics, this age interval has narrowed down. However, you must not delay the operation date later than these months when the child's speech habit is acquired.
1-5 years
The most important feature of this time interval is the development of speech that requires good hearing. Children with cleft palate may have ear problems that can lead to hearing impairment. For this reason, it may be necessary to attach ear tubes to the child. If the scar left by the lip of the lips is not ideal, a scar revision can be made during this period. From time to time, a hole or fistula may develop after repair of the palate. As a result, food and liquids can escape into the nose. This hole can also be repaired in the same period. Ear tube and scar revision can be performed in the same surgery.
5-13 years
Children with a cleft palate may have problems with crowding and gums. Orthodontists, after the age of 5-6 use a variety of tools to fix the teeth. Bone grafting may be needed to support dog teeth during this period, to provide support to the nasal floor and other teeth. This procedure is usually performed with bone fragments from the hip bone. Despite the treatments, if the child's speech is problematic, it can be corrected with an operation called pharyngoplasty. This surgical procedure helps smooth out the sounds from the narrow back of the throat.
13-18 years
In this period, operations for skull revisions, rhinoplasty (nose correction) and jaw surgery to correct crowded teeth are carried out. Rhinoplasty and jaw surgery can be performed when facial development is complete. The ideal time for this is between 16 and 18 years old.
Embedded Teeth
An adult person has a total of 32 teeth, 16 of which are on the top and 16 are on the bottom. Each tooth comes from two parts, the kuron and the root. Kuron produces the part of the tooth visible in the mouth while the roots form part of the tooth that is firmly attached to the jaw. The gum clings firmly to the neck of the tooth and covers the bone holding the teeth. The minor teeth are located in the posterior regions of the mouth and can be 2 or 3 rooted. Most of the other teeth are single-rooted. The last twenty teeth of the minor teeth are the last teeth in the mouth. There are usually four wisdom teeth on each side of the mouth, one at the bottom and the other at the top. These are the teeth that are the most backward of the mouth, so even in the right position they are the hardest to reach and clean.
The jaws most commonly buried in the jaws are wisdom teeth and canine teeth. Wisdom teeth begin to form in a small cavity that develops in the lower and upper jaw. Jaws complete their growth at approximately 16-17 years of age, and at this time, it can be determined whether there is enough room for wisdom teeth to continue normally in the mouth. If there is not enough room for the wisdom teeth to drive, these teeth will be trapped in the area they are in. This is termed as "embedded wisdom teeth". Embedded teeth can stay in many positions while digging downwards. Sometimes some of the embedded teeth may appear in the mouth. Such teeth are also called semi-embedded teeth.
What Type Problems Can Embedded Teeth Cause?
Embedded teeth can cause many problems even if they dont show in the mouth. Patients usually go to the dentist with pain in the back of the jaws or in the ear area. The problem is usually solved by removing the embedded tooth or teeth that cause pain.
There are always bacteria in the mouth. These bacteria can move down the gums and even if you do not see them in the mouth, they can cause a painful infection around the buried tooth follicle. While trying to drive the buried teeth, repeated pain may occasionally occur in the gum covering the buried tooth. If this condition is not treated for a long time (ie the implanted tooth is not removed), the infection can become chronic and cause bone destruction around the implanted tooth. This bone breakdown can also spread around the other teeth behind the mouth, which can lead to forward tooth loss. Bacteria responsible for infectious diseases can cause cavities and cavities in the roots of other molar teeth. Continuous pressures that the embryo teeth bring to the field can cause destruction at the adjacent tooth roots. Cysts and tumors can also occur around the embedded teeth. Other than that, orthodontists may want to remove the implanted teeth because they cause the other teeth to collapse even if they do not create any problems. In addition to all these, an infection from buried teeth can cause problems in the vital organs in the more remote parts of the body. Finally, embedded teeth often occupy an area that must be filled with bone on the lower cannon, which can cause jaw fractures.
When should the implanted teeth be removed?
The moment when wisdom teeth are expected to be buried, they can be removed. This can usually be detected at the age of 16-17, when the jawbone reaches its adult size. There are many benefits of removing the buried teeth at these ages. First, even if the teeth are completely buried at this age, their roots are not fully formed and the bone around the teeth embedded in these patients is more flexible. For this reason they can be removed with an easier surgical procedure. At the same time, post-operative recovery at these ages will be faster.
How to Remove Embedded Teeth
Wisdom teeth can now be easily removed under local anesthesia without any pain in the jaw surgery clinics.
Dental Implants
What is a Dental Implant?
Implantation refers to a medical device placed instead of a missing body part. Implants are typically made of materials compatible with the body (especially titanium). These substances are not considered foreign by the body. So the body does not reject them.
The dental implant term defines a dental device that is placed in place of missing teeth or the root part. These artificial roots can be used as a foundation for the natural appearance of the teeth. In cases where there is loss of some or all of your natural teeth, it allows the patient to safely speak, laugh, chew the food better and more comfortably.
Who can apply dental implants?
Anyone who has lost one or more teeth, or even a portion of the jawbone, is advised for dental implants. Some or all of the teeth are not innate individuals. There are two factors that will affect the outcome of the treatment: one is the the health of the patient. If there is no systemic disease affecting wound healing in the negative, it should be under control. For example, dental implants can be administered in controlled diabetes. However, dental implant application may not be preferred if the patient's condition is unstable or other systemic diseases, such as osteoporosis, are involved. Dental implant therapy should be delayed until the patient's condition is corrected. The other factor : it is necessary to have bone in sufficient quantity and quality to be able to place the implant. When the tooth is lost, the bone around it slowly disappears and reshapes. This way, the bone loss is physiological. If the degree of bone loss is unimportant, implants can be placed, usually without additional procedure. However, advanced bone surgery may require advanced surgical techniques such as bone elevation and / or widening to allow implant placement.
How to Place an Implant
Implant placement in the jawbone consists of two simple surgical procedures. These procedures are simple and usually performed under local anesthesia. The first is to create a nest within the jawbone where the implant will tightly screw and place the implant in the nest. The implant remains buried in the jawbone for 4 or 6 months throughout this healing phase, implant and bone defect. Depending on the type of implant, it remains in the jawbone by being closed or left open. During this time, you can use your current prosthesis or temporary crown-bridge. When the implant is firmly attached to the bone, healing heads are attached to open a second surgical procedure to provide healthy and aesthetic gum formation around the implant neck. At this stage, your prosthesis specialist will select and place the top structures to which the teeth will be affixed, and at the same time prepare the appropriate crown-bridge or restoration type.
There are also special cases for implant preparation. For example, in some cases the implant can be placed in the same seam as the tooth extraction. In order for the implants to be placed in this way, there should be no infection of the dental tooth and enough bone must be available to allow for initial stabilization of the implant. The advantage of this is the shortening of the treatment duration. However, in the majority of cases, it is necessary to wait until the implant cavity heals within 2-3 months before implant placement.
If you are an implant candidate your doctor will discuss this with you. In addition, the patients who are very anxious and predicted to stay operated a long time can be sedated or undergo generalized anesthesia.
Are the implants successful?
Implants are expected to remain functioning for years in patients who have dental implants done. The success of an implant is directly related to a number of patient factors such as the amount and quality of the bone present when the implant is placed, the type of restoration, the type of implant placed, the systemic state of the patient, the experience of the implanting physician, and most importantly, the patient's oral hygiene.
As a result, dental implants are a reliable alternative to dental loss patients and have proved to be an important element in improving quality of life by improving the physical condition of patients.
Cysts and Tumors
Cysts
Cysts are caused by infection in teeth, impairment of rubbing, residual epithelium, etc. When the cysts are examined in two groups as tooth-welded and non-welded, they are usually the most common cause of untreated infections. Another reason is buried teeth. Cysts are widespread due to bone breakdown and can reach very large sizes if not noticed. They need to be removed when they are noticed. They are usually easy to remove because they are encapsulated. The procedure is performed under local anesthesia at the local level, depending on the size of the cyst and its position in the jaws. Procedures for reaching and removing the cyst are performed through the mouth, and after removal of the cyst, the tissues are closed with the suture in their normal position. The proposals to be made after the procedure are intended to make the recovery period as smooth as possible. In some cases, it may be necessary to remove the cyst in the affected teeth.
Tumors
During the development of the jaws, residual epithelium within the bone grows for some reason to form tumors over time. In some cases they can reach very large sizes without causing any symptoms while giving evidence as a cause of pain and bloating. Tumors may be benign or malignant due to the character they originate from. In the treatment of benign tumors, there are options such as removing only the tumor, removing the tumor together with the surrounding bone tissue, or the like. In the treatment of malignant tumors, the bone and surrounding soft tissue in which the tumor tissue is located is completely removed and also the surrounding soft tissue must be removed. Some lymph nodes around the treatment of tumors also need to be removed.
Orthognathic Surgery
Orthognatic surgery is a treatment jointly planned by oral, dental and jaw surgeons and orthodontists. The orthodontist applies a pre-treatment to optimize the post-surgical relationships of teeth and jaws. Sorting teeth in the right position is possible at all ages, often difficult because of the development of the jaw development in advanced age. For this reason, treatment of patients who are approximately 18 to 20 years old, but who have one or both of the jaws may not be possible only with orthodontic treatment. The treatment of a patient at this stage can only be rectified by a surgical procedure. However, patients who require surgery at an early age and who are scheduled for orthodontic treatment may be eligible. This process has recently produced positive cosmetic changes in the function and aesthetics of the patients.
Who needs orthognathic surgery?
Patients without suitable jaw closure and jaws not properly positioned may benefit from orthognathic surgery. Jaws develop slowly and gradually. Jaw damage can occur in jaws for a number of reasons, including birth trauma and genetics. Lower and upper jaws can develop at different rates. As a result, there may be various problems affecting chewing, speaking, oral health and appearance. Orthognathic surgery is a surgical procedure that corrects the functional and / or aesthetic appearance of these patients. Many patients report that their teeth are not fully closed and therefore have difficulty eating and speaking. However, according to our clinical experience, a large percentage of orthognathic surgery patients are very interested in their own aesthetic appearance from the function, complaining that the lower and / or upper jaw is far ahead or far behind. This aesthetic problem can cause problems for most patients in obtaining a social environment. If they are not treated, it is inevitable that some psychiatric disorders will occur in the future. However, very rarely, some patients are not complaining at all. On the contrary, they may think that such a view gives them a distinct character. So it is very important for us that the patient is willing to do this when choosing orthognathic surgery patients.
Some situations that may require orthognathic surgery:
- Difficulty in chewing or biting foods
- difficulty in swallowing
- Speech problems
- Chronic chin pain
- Extreme wear of the teeth
- Open closing (gap between the front or rear teeth when the mouth is closed)
- Irregularity in face appearance
- Birth defects
- Lips that can not touch each other
- Chronic breathing in the mouth
- Sleep apnea etc.
With orthognathic surgery:
- Jaws can be moved forward or backward
- The jaw can be corrected
- The asymmetry of the face can be corrected by gradual bone extension (distraction).
If you are an orthognathic surgeon, you need to be evaluated by an orthodontist or chin surgeon.
How is surgery done and planned?
The patient must be assessed in order to decide the first treatment to be done. First, you should learn what the patient expects from your treatment. Completion of treatment can last from two months to two years. After preliminary information is given to the patient, various measurements are made before the operation. For this, face measurements, photographs, radiographic examinations and study models should be obtained. A complete medical history (questioning) is taken to know if you have any health problems. Any health problem can harm the treatment process. Through anamnesis, it will be determined whether there will be any changes in your treatment depending on your health. Once all this is done, it can be understood that the problem can be corrected by orthodontic treatment. If orthognathic surgery is decided, your orthodontic treatment will continue before surgery and after surgery. Orthodontic treatment usually takes 6-18 months after surgery. At this stage you will visit your orthodontist regularly. After the orthodontic treatment is finished, you may need to use a restraining appliance so that your jaw closure does not get back to its previous state. Your surgeon will receive your new records, including radiographs, measurements and new models, while your orthodontic operations before surgery continue. The oral, dental and maxillofacial surgeon will use these records to estimate the outcome of the surgery and to apply the surgical procedure as planned.
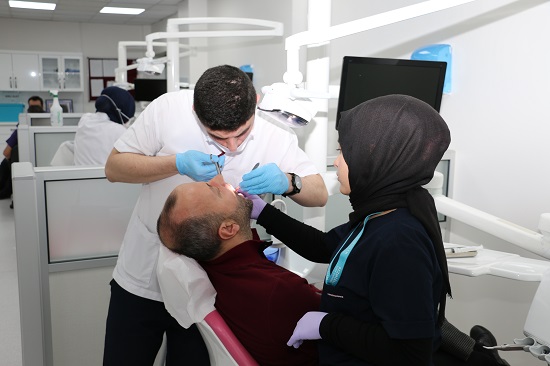
Your surgical procedure will be performed in a hospital environment under general anesthesia. A general check will be carried out before surgery to make sure your health is good. Laboratory tests and various tests will be requested and evaluated. You will need to see an anesthesiologist for evaluation. Before surgery you will be given medications for your relief. The necessary medications and fluids will begin to be delivered by vascular access. While the anesthesiologist manages general anesthesia, your surgeon will carry out your surgery together with your team. After the surgery is finished, you will need to connect a monitor, which is used to monitor your general condition, in the maintenance room. In the meantime, continue to receive fluid through the veins, antibiotics, pain killers, anti-edema and gastric protective drugs will be given to prevent infection. You can stay in the hospital for 2-4 days depending on the type of surgical procedure and your general condition. Your jaws will be connected with wires and tires for 15 days or more to be healed and partly immobilized. You may lose weight because you will feed on a liquid diet during this period. But this is temporary. The first healing period after surgery is 6 weeks. But it can take 9-12 months for a full recovery to take place. Your orthodontist begins orthodontic treatment to improve your closure within about 6-8 weeks after surgery.
Generally, orthodontic wires in your teeth are removed in 6-12 months following surgery. During this treatment you will need to continue to see your general dentist for cleaning and general controls. Other routine dental treatments can be performed during this time.
Surgery can take several hours, depending on the type of treatment to be performed. With surgery, the jaws and therefore the teeth can be shifted forward or backward as far as necessary. Rarely, for certain movements, the jaws can be split into several pieces, adding or removing bones. In most cases, incisions are made through the mouth and there is no visible scar on the outside. As noted earlier, this procedure creates surprisingly positive cosmetic changes in the function and aesthetics of patients and is easily tolerated by patients despite the stress of being operated.
Preprothetic Surgery (Pre-Prosthetic Surgery)
As a result of pathological or physiological changes affecting the tissues in the oral cavity, making an ideal prosthesis is difficult. In addition, some individuals prefer to use their teeth instead of treating them.
A large percentage of the population in our country is not satisfied with current prostheses. Because in the majority of these patients, the amount of bone needed to support the prosthesis is reduced. Today, a variety of surgical procedures are being undertaken to bring such jaws which are unsuitable for prosthetic construction into the ideal anatomical state. These procedures are called "preprosthetic surgery = pre-prosthetic surgery". These include operations such as vestibuloplasty operations, correction of high muscle attachments and frenilums, removal of structures such as unstable krets, tuberocytes, inflammatory papillary hyperplasia, epulis fissuratum, lowering of the mouth base, removal of alveolarplasties, bone exotherms, crest augmentation, dental implant applications etc. to increase the amount of prosthesis. The ideal treatment for such patients can only be given in combination with prosthetic specialists and oral surgeons.
Patients who are difficult to apply prosthesis are older than others. But very few of them need a comprehensive surgeon. The earlier the patients apply for treatment, the better the result will be. Successful surgical treatment also provides a satisfactory relationship between the physician and the patient. Surgical techniques available today make it possible for almost every patient to wear prostheses comfortably and gladly.
Long-term treatment planning must be done before any intervention in soft tissues. The soft tissue, which seems too much at the beginning, can be very useful and useful for operations such as bone augmentation to be performed in the future or keratinized tissue around the implant. However, if the tissue to be removed is thought to be pathological, pathological examination should be performed after the tissue has been removed.
As a result, the preprotic surgeon is based on providing sufficient aesthetic and function with minimal damage to the patient.

Temporomandibular Joint Problems
Temporomandibular joint is the connection point of the lower jaw to the skull base and has a more complex structure than the other joints in the human body. If you put your fingers in front of your ears on the side of your face and open and close your mouth, you can feel the movement of the lower jaw in the TME. When lower jaw is opened, hinge and sliding movements are performed together. There is a cartilage structure called 'articular disc' extending between the bones forming the joint (mandible head = condyle and head base = articular fossa). This dyskinetic movement is controlled by anatomic structures called retrodiscal ligaments and lateral pterygoid muscles that adhere to itself. There is a synovial fluid between the disk and the bony structures that allows it to move freely within the dyskin joint.
Findings related to TME disorders
- pain in TME during jaw movements
- Jaw locks
- Restriction on opening mouth
- Facial aches
- Sounds in TME
Secondary symptoms associated with TME disorders
- Ear pain
- Feeling full of ear
- Headaches
- Tinnitus
- Neck-shoulder pain
Frequently Asked Questions About TME Symptoms
What is the jaw lock?
Locking in the jaw joint is interrupted when the jaw is opened or closed. The patient moves the jaw to the left or right to complete the movement, or it helps to move with his own hand. This occurs when the disc is trapped in the wrong place and prevents the movement of the condyle head. If continued and untreated, damage may occur in tissues that control the joints and articular discs. In severe cases, it may be necessary to perform the procedure under general anesthesia.
What is the limitation in opening the mouth?
If you can open your mouth as wide as you can and place the last three fingers of your hand (middle, ring, sparrow) vertically between the lower and upper teeth, and you do not feel pain and tension at this time, you have normal mouth openness. In general, two fingers or less suggests that there is a restriction on opening the mouth.
My 4 Fingers Fit, What's That Meaning?
Either you have thin fingers or you have extreme mobility on your joints. If you do not have any pain or other complaints, the situation can be considered normal.
I can only place two fingers. Does that mean I need treatment?
This depends on many different factors. What is important is how much this affects your quality of life. If you do not have pain and the only symptom that you have a limitation in mouth opening is that you do not need any treatment. However, your doctor may still want to follow your case.
I hear voices in my TME when I move my chin. Sometimes this is in a click-cracking style, sometimes in a jumping style. What does this mean?
The presence of joint sounds during jaw movements indicates that the functional elements are not working properly. Click-cracking noises are called crepitation (friction) and are associated with bone tissues that contact during this movement. Normally, the condyle head is expected to move with the disc in the joint fluid. For many reasons, the harmony of the condyle head and the diskinous movement is distorted and a jumping sound is heard during mouth opening. After a while, when the mouth is opened and closed, the disc is lost to its normal anatomical position and is transported to another side and crepitation may occur due to rubbing of the bone surfaces or very small surface erosions on the condylar disc surface.
Is the presence of these joint sounds too serious?
If there are no other symptoms, it may not be serious. However, these noises indicate that the joint does not function properly and micro-trauma occurs in the joints as a result of each noise. This means that the TME can develop in the course of time. If you hear these noises during chin movements, you should consult your family dentist or an oral and maxillofacial surgeon who you regularly go to.
Why does the ear sign occur in relation to the TME condition?
Ear tissues are very close to TME. In appropriate X-ray films, TME is closely related to tympanic bones (ear bone). Even if there is not a significant problem at the ear, there may be ear pain, one or both fullness or weight feeling, and sometimes tinnitus in relation to TME problems.
Treatment
Diseases affecting the temporomandibular joint are similar to those affecting other joints in the human body (such as rheumatoid arthritis and osteoarthritis, inflammation of the joint capsule and synovial fluid, tearing or perforation of ligaments or arthritic discs, internal disturbance of the disc or condyle head of joint space). Today, different methods of treating TME diseases are applied:
- Soft diet
- Bite plates
- Stress treatment
- Medication
- Physiotheraphy
- Surgical treatment
Treatment planning for TME disorders should be based not only on the removal of existing symptoms but also on the patient's need and desire. For example, click sound may not require treatment for all patients. Surveys show that about 50% of people face this noise at any time of their life.
As a result, all treatment modalities should aim at providing a function of the jaw at an acceptable level and eliminating symptoms such as pain from affecting the patient's social life.
Trauma
After the trauma that will occur in the jaw face region, a wide range of different fractures can occur in the range from the most simple tooth fractures to the fractures of much larger jaw face bones. Trauma is usually caused by traffic accidents, sports injuries, fighting, falling, etc. for reasons. The most basic condition of the trauma is the injury limited to the tooth. Until the tooth breaks out completely from the tooth cavity, different results may occur. In more severe traumas, fractures can occur in the alveolar bone where the tooth is placed together with the tooth. In this case, according to the condition of the fracture, the fracture of the tooth can be treated with filling materials, it can be fixed to the neighboring teeth by placing it in place, and if the alveolar bone is broken, it can be fixed with various methods of bone.
In larger trauma cases, In the case of fractures and fractures involving the cheekbone, lower jaw or all, it is first necessary to fully understand and evaluate the condition of the fractures. Panaromic films and dental tomography are used for this purpose. After the condition of the broken parts is evaluated, the processing to be carried out will be decided. If there is no movement in the fractured parts, fracture can be treated by connecting the upper and lower jaws for a certain period of time. If there is incompatibility between the broken parts and there is no ideal closing with the connection of the jaws, the fracture line must be opened by operation and fixed to the original position with plates and screws.